Perthes disease
Perthes disease is a rare condition affecting children, in which blood supply to the “ball of the hip joint” (femoral head) is temporarily disrupted. This disease process in Perthes usually lasts 2-3 years and is self limiting (means, it stops by itself without any treatment).
You may be thinking why we are worried about a disease which is self limiting and not life threatening! By the time Perthes comes and goes, it damages the structure of bone (this process is called avascular necrosis) resulting in loss of shape of the ball. This abnormal shape persists throughout life and may even worsen. It is easy to understand that any change in smooth shape of the joint can lead to early wear and tear (osteoarthritis hip) of it. This results in a painful joint in the prime age of the person (40s), which limits his activities and is usually treated with a major total hip replacement surgery.
Treatment for Perthes focuses on preventing the ball of hip joint from losing its rounded shape or helping it to grow back into a shape that still fits into the socket of the hip joint. This will help the hip joint move normally and prevent hip problems in adulthood.
The long-term result for children with Perthes is good in most cases. After 18 to 24 months of treatment, most children return to daily activities without major limitations.
Perthes disease typically occurs in children who are between 4 and 8 years old. It is five times more common in boys than in girls. In 10% to 15% of the cases, both hips are affected.
Cause
No clear reasons behind the occurrence of Perthes disease are found so far. Researchers could make only some suggestions about its causation:
1) Decreased blood supply of femoral head (This is probably seen in all children during the age 4-8 years)
2) Injuries to the hip can cause swelling within the joint which can worsen the already compromised blood supply of the joint.
3) Hyperactive children are more prone to get this condition
Symptoms
1) Limping: One of the earliest signs of Perthes is a change in the way the child walks and runs.
2) Pain in the hip or groin, or in the thigh or knee
Symptoms may come and go over a period of weeks or months before parents consider a doctor visit.
Doctor Examination
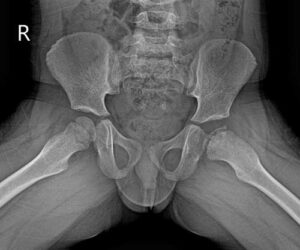
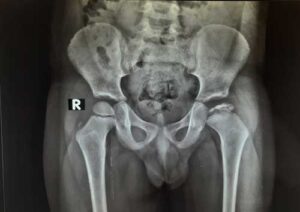
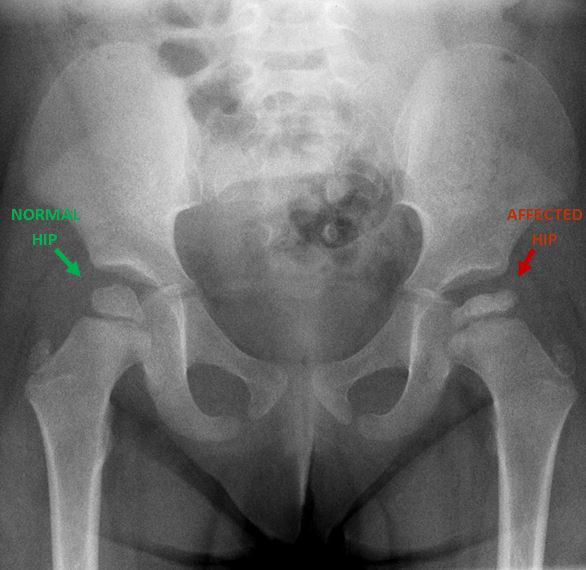
After discussing your child’s symptoms and medical history, your doctor will conduct a thorough physical examination and take x rays of the hip. Usually 1-2 x rays are adequate to make the diagnosis of Perthes disease, but sometimes confirmation diagnosis or treatment planning may need MRI scan of hips.
A child with Perthes can expect to have several x-rays taken periodically over the course of treatment. As the condition progresses, x-rays often look worse before gradual improvement is seen.
Treatment
The goal of treatment is to relieve painful symptoms, protect the shape of the femoral head, and restore normal hip movement. If left untreated, the femoral head can deform and not fit well within the acetabulum, which can lead to further hip problems in adulthood, such as early onset of arthritis.
There are many treatment options for Perthes disease. Your doctor will consider several factors when developing a treatment plan for your child, including:
* Your child’s age.Younger children (age 6 and below) have a greater potential for developing new, healthy bone.
* The stage of disease at the time your child is diagnosed.How far along your child is in the disease process affects which treatment options your doctor will recommend.
Nonsurgical Treatment
Observation- For very young children (those 2 to 6 years old) who show few changes in the femoral head on their initial x-rays, the recommended treatment is usually simple observation. Your doctor will regularly monitor your child using x-rays to make sure the re-growth of the femoral head is on track as the disease runs its course.
Anti-inflammatory medications- Painful symptoms are caused by inflammation of the hip joint. Anti-inflammatory medicines, such as ibuprofen, are used to reduce inflammation, and your doctor may recommend them for several months. As your child progresses through the disease stages, your doctor will adjust the dosage or discontinue the medication.
Limiting activity- Avoiding high-impact activities, such as running and jumping, will help relieve pain and protect the femoral head. On occasion, your doctor may also recommend crutches or a walker to prevent your child from putting too much weight on the joint.
Physical therapy exercises- Hip stiffness is common in children with Perthes disease and physical therapy exercises are recommended to help restore hip joint range of motion.
Casting and bracing- If range of motion becomes limited or if x-rays or other image scans indicate that a deformity is developing, a cast or brace may be used to keep the head of the femur in its normal position within the acetabulum.
Petrie casts are two long-leg casts with a bar that hold the legs spread apart in a position similar to the letter “A.” Your doctor will most likely apply the initial Petrie cast in an operating room in order to have access to specific equipment.
Surgical Treatment
Your doctor may recommend surgery to re-establish the proper alignment of the bones of the hip and to keep the head of the femur deep within the acetabulum until healing is complete. Surgery is most often recommended when:
* Your child is older than age 8 at the time of diagnosis. Because the potential for deformity during the re-ossification stage is greater in older children, preventing damage to femoral head is even more critical.
* More than 50% of the femoral head is damaged. Keeping the femoral head within the rounded acetabulum may help the bone grow into a functional shape.
* Nonsurgical treatment has not kept the hip in correct position for healing.
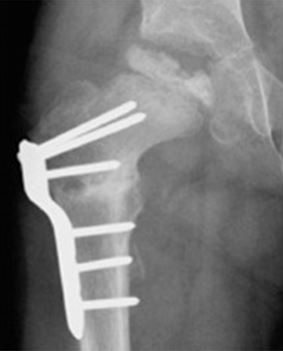
The most common surgical procedure for treating Perthes disease is an osteotomy. In this type of procedure, the bone is cut and repositioned to keep the femoral head snug within the acetabulum. This alignment is kept in place with screws and plates, which will be removed after the healed stage of the disease.
In many cases, the femur bone is cut to realign the joint. Sometimes, the socket must also be made deeper because the head of the femur has actually enlarged during the healing process and no longer fits snugly within it.
Outcomes
In most cases, the long-term prognosis for children with Perthes is good and they grow into adulthood without further hip problems.
If there is deformity remaining in the shape of the femoral head, there is more potential for future problems; however, if the deformed head still fits into the acetabulum, problems may be avoided. In cases where the deformed head does not fit well into the acetabulum, hip pain or early onset of arthritis is likely in adulthood.